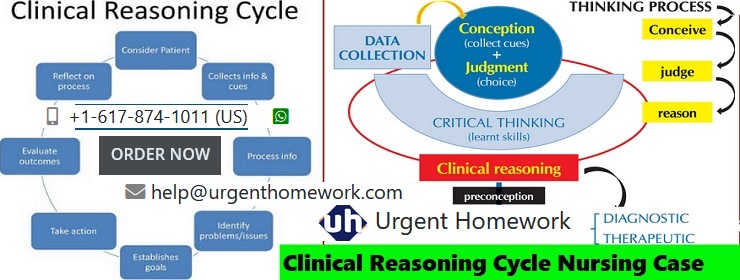
Clinical Reasoning Cycle
Clinical Reasoning Cycle in Nursing Case Study
Clinical Reasoning Report CNA155 Assessment Case Study: John Wells Background: John is an 82 year old dairy farmer brought in the emergency department by his son, Sam. Sam received a call from his mother Mavis, as she was concerned about her husband. Mavis noticed that John appeared somewhat quiet, and hasn’t eaten his dinner tonight. John had told Mavis that he was returning home from the dairy for morning tea, pulled up outside their home on the two-wheeled motorbike and became unbalanced. The bike was stationary at the time and John fell clear of the bike, striking the left side his head on the hard summer ground. John rarely wears a helmet, or any other protective equipment when he works on their property, and today he wasn’t wearing any. John has sustained a minor skin tear to his left forearm and small abrasion to his left elbow. John denies any other injuries and denies pain, stiffness or reduced range of movement to his neck, chest and limbs. Mavis was concerned about John, so she asked Sam to take John to the hospital.
Consider the patient:
82-year-old farmer with no previous history of head injury or concussion. He is usually well, diagnosed with mild hypertension but not yet prescribed antihypertensive medication. John is local to the rural area where he resides, lives with his elderly but otherwise well wife. John and Mavis’s only son Sam lives on the neighbouring property. John and Mavis value their independence, and Sam is usually happily able to assist his parents if required.
Patients notes: Emergency Department
82-year-old male brought to the emergency department after experiencing headache, nausea, and mild confusion after hitting his head following a fall from a stationary motorbike. Currently states he is ‘feeling hazy’ and complains he is experiencing a headache 4/10. He states he was initially ‘dizzy’ after hitting his head and denies losing consciousness. He states he is ‘just not feeling right’.
John Vital Signs:
Temperature:36.7 degrees Celsius
Blood pressure: 148/84 mmHg
Pulse: 81 bpm
Respiratory Rate:17 bpm
SpO2: 97% on room air
Assessment Task:
- Consider the patient situation: Discuss what is significant about the patient’s profile making links to how you think this information relates specifically to the situation. It is critically important that you discuss John’s risk factors.
- Collect cues and information: Review the patient’s notes from both the emergency department and the information prior to presentation. Note the subjective and objective data, differentiate normal from abnormal. Also, indicate the potential significance of any changes you identify. Propose new assessment data/cues to collect, and describe the nursing assessments that you will use to collect those cues, as well as the frequency with which those assessments might need to be performed. Link the nursing assessments to a clear understanding of what is occurring from a functional and structural perspective within the brain. Making these links requires you to recall knowledge of the scientific principles underlying the case.
- Process the information, relate, and infer: Cluster the cues in the case to identify and support a problem that you think maybe occurring with the patient. From what you know about John’s background, the cue s you have clustered, and the sign and symptoms he is experiencing, explain your interpretation of his condition. In other words, what do you think is going on?
Clinical Reasoning Cycle in Nursing Case Study Answers and Solutions by Urgenthomework
Introduction:
Whilst of many similarities in the process, nurses and different health specialists believe, also hold notable distinctions. Unlike these health experts who ‘treat’ as well as ‘retreat’, remedial relations among nurses as well as their subjects could prolong beyond minutes, days or even longer. Nurses are thus supposed to take care of and execute determinations regarding disordered patients having a range of health requirements. Clinical reasoning is a methodical as well as a cyclical method that helps in making decisions based upon clinical practices especially in random, developing, and specific conventional conditions, which then helps in making the right and familiarized clinical experiences. Clinical rationalizing abilities leave a positive effect upon inpatient consequences whilst, on the contrary, nurses having inadequate clinical rationalizing abilities tend to fail usually in the detection of patient degeneration, leaving to recover. The process of clinical reasoning commences at 1200 hours and proceeds in a clockwise orientation in eight stagings which are: view, gather, process, diagnose, design, perform, assess, and reflect. Though the individual stage is exhibited to be essentially a separate and discrete component, in actuality, clinical rationalizing is considered as a progressive method where nurses usually connect one or more staging or sway back and forth amidst them ere arriving upon an investigation requires adequate actions to take place and assessing the consequences (Levett-Jones, 2017).
Consider the patient situation:
A neurological review evaluates the patient's motor and sensible abilities, sound and language, perception, coordination, as well as stability. In addition, it might ask to conduct a test of their psychic state, condition, and performance. The research utilizes instruments like a tuning fork, spotlight, reflex hammer, and a device to examine the eye. The effects of both, the neurological exam as well as the history of the patient are practiced in determining a shortlist of circumstances, perceived as the differential analysis, which assists in determining supplementary symptomatic examinations and methods if required (Ninds.nih.gov, 2019).
To assess the patients’ risk factors, it is vital to evaluate some tests such as the patients’ consciousness level according to the Glasgow come scale (CGS); the traditional vital signs; observations regarding some focal signs like- the size of the pupil and the reaction and to see if there is any movement present in the limbs or not.
The scores of these signs would thus help us to evaluate further treatment options.
Neurological examination is important in case of any head injury and these following measures must be noted down like the patient’s: Level of consciousness; how much he is verbally responding; motor skills he would be responding to and the status of his vital signs like the temperature; blood pressure; pulse rate and respiration rate.
The status of every category is essential to note down if he is doing the best or giving a poor response towards the examinations conducted as it would lay an impact upon the further assessment to be undertaken (Observations Neurological, 2010).
In the case of John, the vital signs are quite normal with a slight abnormal blood pressure which would come to normal with rest, and when he got hit, he felt slight dizziness with no loss of consciousness, and right now, he is feeling hazy that means his level of consciousness and motor skills would be tested. His verbal test would be analyzed along with his ability to open his eyes.
John is 82 years old; age plays a significant role in deciding the recovery from the disease. Higher the patients’ age more the problem gets complexed to even when signs showed by the patient earlier do not indicate any disease. As hypertension is indicated by John’s chart age plays a significant role in this (Chowdhury et al., 2014).
Sex does not play a significant role in determining the susceptibility to get neurological damages. Whether it is a male or female, the differences come from social interactions that is the type of environment they live in and their surroundings (Jäncke, 2018). However, during research, it has been found out that neurological disorders such as Parkinson’s, migraine, epilepsy, multiple sclerosis, female have shown more adverse drug reactions (Clayton, 2016). So, John, in regards to this factor does not impose a risk to manifest any neurological disorder.
As John lives in a rural area, he must be less knowledgeable about the neurological disease and would tend to be more slurred (Elliot et al., 2018).
Over 65, the diet must be changed and it should be more inclined towards eating healthy and fresh else the chances of having CVD’s or mental health issues like anxiety, fear, depression increases. A wide variety of food must take with the least saturated food intake. Plenty of water must be taken. Alcohols, extra salt, and sugars must be limited to a great extent. Short meals with high calories for men is recommended. Calcium is vital in the regular diet for strong bones (Betterhealth.vic.gov.au, 2019). In the case of John, these precautionary measures must be followed strictly as his wife reported that he has not eaten his meal and went to work. Skipping of meals must not be tolerated at his age.
Collect cues and information:
As John never wears any precautionary gadgets while or after working it increases his susceptibility to getting the injury with more severity. On his body, there have been minor scratches that would eventually heal with time and do not require much medical concern. He showed signs of being hypertensive but no medication was recommended for that course. But his neurological conditions might need some attention as when he hit the ground, he reported that he felt dizziness, and the emergency department reports headache, nausea, mild confusion accompanied by a feeling of haziness. His vital signs show some fluctuated levels that tend to be stabilized in the normal person. With this information, it would be recommended to have GCS inclusive of test for eye-opening (spontaneous/ pain/ speech or touch or nil), verbal expression (spontaneous/confused or no expression), and efficient motor response (holds tightly/ flexible/ loose skill or nil). With each assessment, a specific marking scheme is allocated and accordingly response and management response are decided. However, John did not complain about his reduced movements of limbs, I would be still recommended to examine the functioning of upper and lower limbs by asking him to have active movement against gravity, foot dorsiflexion, etc. whereas upper limbs could be tested by chicken wings, elbow flexion, etc. His pupil size would be noticed upon putting up a torchlight (consensuality of pupil response, reaction to light, equality) and cranial nerve assessments would thus be carried out (Aci.health.nsw.gov.au, 2013). With the increasing age, the nerve cells die and this intends to bring out abnormal changes in the brain leading to the formation of tangles and plaques. With the decreasing number of nerve cells not only waste products will get accumulated in the brain but also it would affect and compromise the activities of the cranial nerves too (Medlineplus.gov, 2019). Since cranial nerves do inform us the functions of motor and sensory nerves of the head and neck basically. So, assessing the cranial nerves by differential tests would let us determine if there is a defect in any nerve or not. With age response and functioning of the nerves do get decreased therefore after an incident it’s a must to test them. Tests such as the sensation of the face, extraocular movements, gross hearing, test for soft palate rise and midline vulva, etc. can be done to analyze the status of the functioning of the cranial nerves of the patient (Aci.health.nsw.gov.au, 2013). These tests are usually conducted to determine the level of consciousness. If the tests are responded to well at the initial stage only then there is no requirement to test them in intervals and if the patient show diminished responses then he must be checked for verbal expression, eye-opening testing and evaluation of motor skills must be done at regular intervals when he is found to be in the state of consciousness.
Process the information, relate, and infer:
By hitting on the ground John may have faced concussions as the signs and symptoms showed by him relate to the conditions leading to acute neurological disturbance. Headaches, nausea, no loss of consciousness, dizziness, or feeling hazy meaning slight confusion are a few of the signs which were shown by John after the incident (Mayo Clinic, 2019). Mild painkillers for the headaches and anti-nausea tablets in case of nausea could be prescribed. A CT scan could be referred to see if there is any internal bleeding. As John, did not show any internal serious injuries he would be asked to have proper bed rest till he gets well. He should resume his heavy activities only after the doctor has recommended. A man of this age should have a proper diet. He must take care of the kind of food he is eating. After the incident, he must start with light meals and moderate water intake. After when he gets recovered properly from his stage, he must plan a diet that encompasses ingredients considering the five main groups that is fruits, vegetables, legumes/beans, meat/ poultry/fish and dairy products. Studies have suggested that a decrease in appetite has been observed, over the age of 65 years (Pilgrim et al., 2015). But John must maintain his diet either in short intervals so that he doesn’t get deficient in nutrition which would result in poor health consequences and slower recovery from the incident. If headaches or difficulty in memorizing or understanding or lack of concentration is faced by John then he must report to the doctors and seek medical assistance because this age demands slower recovery and sometimes proper recovery is not feasible.
Conclusion:
Nurses are required to mature into skilled communicators who exhibit sensitive knowledge within their work setting. To do so, they should acquire critical self-understanding whenever they have interactions and relations with their patients. Self-understanding is the principal medium by which nurses could estimate their efficacy concerning their subjects (Stein-Parbury, 2014). Assessment of the neurological exams is essential in situations where there is a risk of getting a head injury. Early interventions could help in bypassing the adverse outcomes and thus timely effective management could take place. With advancing age not only assessment criteria for such examinations changes but also its treatment and management options incorporating fluctuating patterns in the diet. Thus, a healthy diet is a vital component of healthy living which thus establishes a concept of undertaking a nutritious diet that is void of junk food and high calories and is inclusive of the five main categories of food so that every essential nutrient is consumed by the body. A healthy mind resides in a healthy body, therefore, a better appetite encompassing enriched foods must be ingested.
References
Betterhealth.vic.gov.au. (2019). Nutrition needs when you’re over 65. [online] Available at: https://www.betterhealth.vic.gov.au/health/HealthyLiving/Nutrition-needs-when-youre-over-65
Betterhealth.vic.gov.au. (2019). Head injuries and concussion. [online] Available at: https://www.betterhealth.vic.gov.au/health/ConditionsAndTreatments/head-injuries-and-concussion
Chowdhury, R., Hasan, A., Rahman, Y., Khan, S., Hussain, A., and Ahsan, S. (2014). The pattern of neurological disease seen among patients admitted in tertiary care hospital. BMC Research Notes, [online] 7(1), p.202. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3977680/.
Clayton, J. (2016). Sex influences in neurological disorders: case studies and perspectives. Dialogues in Clinical Neuroscience, 18(4), pp.357–360.
Elliot, V., Morgan, D., Kosteniuk, J., Froehlich Chow, A. and Bayly, M. (2018). The health-related stigma of noncommunicable neurological disease in rural adult populations: A scoping review. Health & Social Care in the Community. [online] Available at: https://onlinelibrary.wiley.com/doi/full/10.1111/hsc.12694.
Jäncke, L. (2018). Sex/gender differences in cognition, neurophysiology, and neuroanatomy. F1000Research, [online] 7, p.805. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6013760/.
Levett-Jones, T. (2017). Clinical reasoning. 2nd ed. Pearson Australia Group Pvt Ltd.
Mayo Clinic. (2019). Concussion - Symptoms, and causes. [online] Available at: https://www.mayoclinic.org/diseases-conditions/concussion/symptoms-causes/syc-20355594.
Medlineplus.gov. (2019). Aging changes in the nervous system: MedlinePlus Medical Encyclopedia. [online] Available at: https://medlineplus.gov/ency/article/004023.htm.
Ninds.nih.gov. (2019). Neurological Diagnostic Tests and Procedures Fact Sheet | National Institute of Neurological Disorders and Stroke. [online] Available at: https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Neurological-Diagnostic-Tests-and-Procedures-Fact.
Observations Neurological. (2010). pp.1-7.
Pilgrim, A., Robinson, S., Sayer, A. and Roberts, H. (2015). An overview of appetite decline in older people. Nursing Older People, 27(5), pp.29-35.
Stein-Parbury, J. (2014). Patient and person. 5th ed.
Essay Topics for Clinical Reasoning Cycle
- Admission Essay writing Service
- Analytical essay
- Application Essay
- Argumentative Essay
- College Essay Help
- Comparative Contrast essay
- Custom Essay Help
- Descriptive essay
- Evaluative essay
- Exegetical Essay Writing Help
- Expository Essay
- Literature Essay
- Narrative Essay
- Persuasive essay
- Reflective Essay
- Research Proposal
- Response essay
- Thesis Essay Writing